The Excess of Sugar and its Relationship with Liver Cancer
At the Marc Bony Chiropractic Center in Mataró, we explore how excess sugar is linked to liver cancer. Learn how to prevent it through natural health.
Excess sugar, chemicals, and liver cancer
Worldwide, hepatocellular carcinoma (HCC) of liver cancer is the second leading cause of cancer death due to its high prevalence and the difficulty of treatment. Researchers warn that by 2030, the global liver cancer rate will double, affecting more than 1.2 million people.
Alcohol-induced cirrhosis and NAFLD (non-alcoholic fatty liver disease) can be reversible in their early stages if you quit alcohol and reduce your processed fructose intake, respectively.
Non-alcoholic fatty liver disease (NAFLD) is becoming increasingly common. Between 2001 and 2013, the number of diagnosed cirrhosis cases nearly doubled, and deaths from cirrhosis increased by 65% between 1999 and 2016. The largest increase (10.5%) was recorded among those aged 25 to 34, where alcoholic cirrhosis has surged.
Excessive sugar consumption drives the rise in NAFLD (Excess Sugar)
While alcohol-related cirrhosis is increasing mortality rates, the growing prevalence of NAFLD is contributing to the overall burden of liver disease. In the case of NAFLD, fatty liver occurs in the absence of significant alcohol consumption and is instead driven by excess sugar, which is now even found in young children.
NAFLD is often asymptomatic, although it can cause fatigue, jaundice, swelling in the legs and abdomen, mental confusion, and more. If left untreated, it can cause inflammation of the liver, called non-alcoholic steatohepatitis (NASH), and can lead to liver cancer or liver failure. However, just as with alcohol-related cirrhosis, NAFLD can be reversed in its early stages by following a proper diet and exercising.
Most importantly, you must eliminate processed fructose and other added sugars from your diet. Fructose affects your liver in ways very similar to alcohol. Unlike glucose, which can be used by virtually all cells in your body, fructose can only be metabolized by the liver as it is the only organ that has the transporter for it.
Since all fructose is transported to your liver, if you consume it in large amounts, it ends up damaging and deteriorating this organ in the same way that alcohol and other toxins do.
Moreover, the way your liver metabolizes fructose is very similar to that of alcohol, as both substances serve as substrates to convert carbohydrates into fat, promoting insulin resistance, dyslipidemia (abnormal fat levels in the bloodstream), and fatty liver.
Additionally, fructose undergoes the Maillard reaction with proteins, leading to the formation of superoxide free radicals that can cause liver inflammation similar to that of acetaldehyde, an intermediate metabolite of ethanol.
According to Dr. Robert Lustig, a neuroendocrinologist in the endocrinology division at the University of California, fructose is a “chronic and intrinsic liver toxin,” meaning it is dose-dependent.
Excess glucose converts to fructose and depletes your NAD+ (Excess Sugar)
The problem is not only consuming excess fructose in processed foods, but ultimately, in an effort to metabolize glucose, the excess glucose is converted to fructose to obtain energy. Let me explain this in more detail.
When your body is exposed to chronic excess glucose, the first enzyme that breaks it down is hexokinase, and when this enzyme becomes saturated, it can no longer break it down.
Once this occurs, glucose will be metabolized through the polyol pathway, where aldose reductase metabolizes glucose into sorbitol, and sorbitol dehydrogenase subsequently metabolizes sorbitol into fructose (see the diagram below).
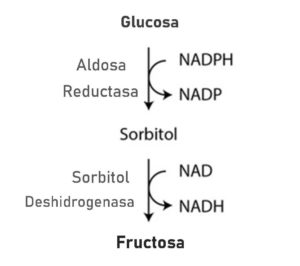
It is estimated that when you are in good health, only about 3% of glucose goes through the exposed pathway, but at least 30% of it flows through this pathway in chronic hyperglycemia, creating a vicious cycle of excess fructose.
This metabolic catastrophe is a redox reaction that results from the exchange of one NADPH molecule for one NADH molecule. This is precisely what should not happen, as NADPH is used as a reserve reducer for your antioxidants and is necessary to produce both your steroid hormones and fats. When your levels are low, you will start to experience severe difficulties.
To make matters worse, it increases your NADH levels and worsens your NAD to NADH ratio. As the fuel supply exceeds metabolic demand, the ratios of mitochondrial and cytoplasmic NAD and NADH decrease. The resulting hyperpolarization of the mitochondrial membrane perpetuates electron leakage and excess oxidative stress.
Fortunately, there is a simple and affordable solution that should radically improve this metabolic catastrophe. The first thing you must do, invariably, is to clean up your diet as we have advised repeatedly, so your body can burn fat as fuel.
However, you can also take NAD precursors like simple extended-release niacin. That should help increase the NAD/NADH ratio and NADPH levels. My recommendation is to start with a dose of 25 to 50 milligrams several times a day, as taking a higher dose will likely cause a harmless but relatively annoying flushing sensation.
It would also be helpful to reduce your exposure to electromagnetic fields, as this also consumes NAD through the hyperactivation of PARP and will worsen the metabolic condition.
Folate, milk thistle, NAC, coffee, and broccoli help promote healthy liver function.
- Folate consumption may also help protect your liver function. In fact, studies have shown that folate deficiency can increase your risk of liver cancer. This nutrient can provide your liver with some degree of protection against damage. Similarly, folate can mitigate pesticide-related damage, including autism.
- Milk thistle is an herb that has been used for thousands of years to promote the health of the liver, kidneys, and gallbladder. In modern times, silymarin has been used to treat alcoholic liver disease, acute and chronic viral hepatitis, as well as toxin-induced liver diseases. The active ingredient, a flavonoid called silymarin, is believed to be responsible for the beneficial effects attributed to milk thistle, including liver protection, antioxidant, antiviral, and anti-inflammatory properties.
- N-acetylcysteine (NAC) is a potent liver protector and a necessary precursor for glutathione biosynthesis. In fact, research suggests that compared to antioxidant resveratrol, NAC is likely a better alternative for supporting liver health in people suffering from hepatitis C and other chronic liver diseases.
- If you enjoy drinking coffee, you may be pleased to discover that it seems to have a protective effect against hepatocellular carcinoma (HCC), a severe form of liver cancer and the second most common cause of cancer death worldwide. Drinking one cup of coffee a day reduces the risk of HCC by one-fifth. If you are interested in optimizing the benefits that coffee provides, drink it black and in its organic version without milk or sugar. Still, it is advisable not to overdo it, as there are at-risk groups such as pregnant women who should avoid it during pregnancy, as suggested in his study by Dr. Oliver Kennedy from the University of Southampton in the UK.
Low-level chemical exposures are linked to liver damage
Although there is no concrete data, there are studies suggesting that today, alcohol-induced cirrhosis is presenting at a younger age as a result of liver damage caused by chemical exposures. In fact, researchers have shown that even small amounts of chemicals in food, medicines, and personal care products can cause liver damage.
One of the aforementioned experiments was designed to evaluate the effects of low-dose chemical combinations whose sources were purely environmental, such as food, medications, and personal care products.
Roundup damages the liver even in minimal doses
Roundup, the most widely used herbicide in the world, has also been linked to liver damage. Alarmingly, glyphosate levels in urine have skyrocketed in the last two decades, suggesting widespread chronic exposure, most likely from food.
Sources and references:
- American Cancer Society 2017
- New York Times July 18, 2018
- gov NCHS Data Brief No. 314, July 2018
- BMJ 2018;362:k2817
- The University of Southampton 2017
- Gastroenterology 2015 Nov;149(6):1471-1482.e5; quiz e17-8
- NPR July 18, 2018
- Washington Post July 18, 2018
- American Journal of Public Health 2015 Jun;105(6):1120-7
- Journal of the American Dietetic Association, September 2010; 110(9): 1307-1321
- Pyridine Dinucleotides from Molecules to Man 2018; 28(3)
- Diabetes 1984 Feb;33(2):196-9
- Food and Chemical Toxicology, 2018;115:470
- GMWatch, June 7, 2018
- Annals of Occupational and Environmental Medicine, 2013;25:5
- World Journal of Gastroenterology, 2012; 18(22):2756
- Carcinogenesis, 2015;36(1): 2254
- Cancer, Epidemiology, Biomarkers and Prevention, 2007;16(6):1279
- 34, 35 Nutraingredients, July 19, 2008
- 36 The World’s Healthiest Foods, Folate
- 37 J Nutr March 2016;146(3):542-50
- 38 BMJ Open 2017; 7(5)
- 39 Medical News Today May 30, 2017
- 40 CBS Philly May 30, 2017


